How To Heal Sore Nipples (The Right Way)
This post may contain affiliate links (see full disclosure). As an Amazon Associate, I earn from qualifying purchases.
Are you experiencing nipple pain while breastfeeding? Not sure what to do? This post walks you through what a lactation consultant (IBCLC) recommends to heal sore nipples.
Sore nipples are one of the most common issues breastfeeding parents experience. So common, in fact, that you might have even been told experiencing nipple pain is a “normal” part of breastfeeding.
Spoiler alert: It’s not.
While it is normal to feel some nipple discomfort in the early days of breastfeeding, it should never become outright painful, and normal discomfort should resolve itself within 1-2 weeks postpartum. Nipple soreness that persists longer than this is often a sign of a latch problem that should be addressed. But let’s talk about how to heal sore nipples (the right way) in the meantime!

Sore nipples with a latch that “looks good”?
Unfortunately, It is extremely common for breastfeeding parents to be told baby’s latch “looks good” in the hospital, only to come home and develop painfully sore nipples. It’s also unfortunately common for breastfeeding parents to hear that latch “looks good” even while the latch is actively causing them pain!
The truth is, we don’t just care about how “good” the latch looks. We also care about comfort, function, and sustainability. In other words, the latch needs to not be painful. It needs to enable baby to effectively get milk out. And if baby can’t stay latched on his/her own (i.e. baby keeps slipping off the nipple unless held in place), then the latch is not sustainable and isn’t going to work.
A latch that causes ongoing pain isn’t a good latch, even if it “looks good.”
So what can you do about nipple soreness? As an International Board Certified Lactation Consultant, I’d recommend the following:
1. Get help sooner rather than later
One of the biggest mistakes breastfeeding parents make is waiting to get help with nipple pain. This is a problem for multiple reasons.
For one, the longer you are in pain, the more draining breastfeeding can start to feel. Unresolved pain can drive breastfeeding parents to quit breastfeeding before they’re ready.
But even if you are determined to continue, untreated nipple pain can still lead to low milk supply. This is because nipple pain is almost always a sign that something is going on with baby’s latch. If baby isn’t able to latch onto the breast deeply, your body may not get the stimulation it needs to keep up milk production over time. So it’s best to correct poor latch—and rule out other obstacles to breastfeeding—before these things become a problem.

If possible, I recommend setting up an appointment with a lactation consultant around 4-5 days postpartum—even if things seem to be going well. Private practice lactation consultants often meet with you in the comfort of your own home, and they usually meet with you far longer than hospital-based lactation consultants are able to work with you in the hospital. Many lactation consultants take insurance or can provide you with the information you need to get insurance to reimburse you for the visit.
If needed, free breastfeeding help can also be found through peer support organizations like La Leche League or Breastfeeding USA. If you’re having trouble finding lactation help, please feel free to contact me and I will do my best to help you find care in your area.
READ MORE: How To Find A Lactation Consultant Who Supports You
Important Note: Pediatricians are often the first people breastfeeding parents turn to when they are having trouble breastfeeding, but most pediatricians do NOT have professional lactation training. Lactation care is NOT a routine part of a pediatrician’s training. Pediatricians who do have lactation training may not be able to spend as much time working with you as needed. As a result, pediatricians are often NOT the best resource for lactation care. A breastfeeding-friendly pediatrician will most likely refer you to an IBCLC rather than try to manage your care themselves.
2. Adjust baby’s latch
Correcting a shallow latch is probably the most effective way to heal sore nipples long term.
A shallow latch can cause nipple pain for a few reasons. First, If not enough of the breast is pulled into baby’s mouth, baby’s tongue will rub against the face of the nipple, causing nipple abrasions and tissue damage. With a deep latch, baby’s tongue will rest underneath the nipple instead.
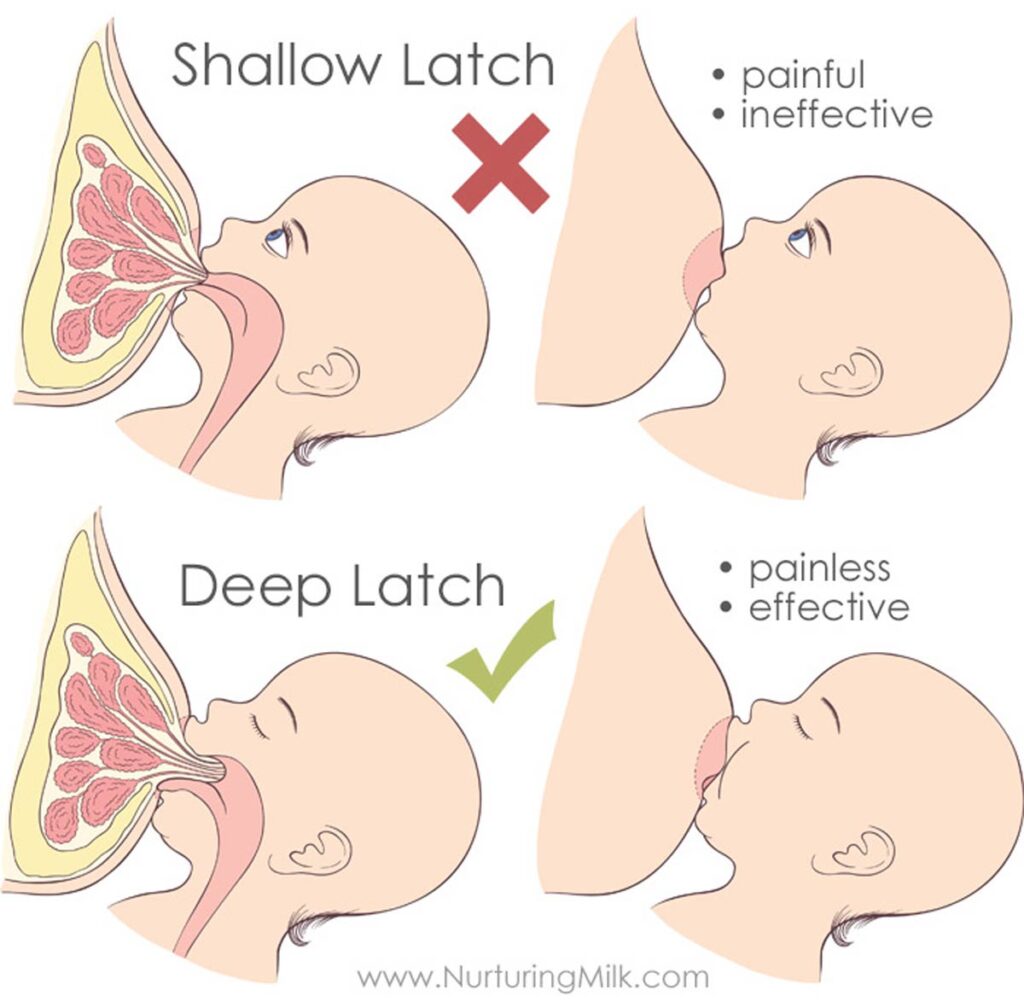
Furthermore, if the nipple isn’t deep in baby’s mouth, it may be crushed by baby’s hard palate, causing pain. With a deep latch, the breastfeeding parent’s nipple is pulled back far into baby’s mouth, where it is instead gently compressed by baby’s soft palate.
It makes sense, then, that one of the best ways to resolve nipple pain would be to make sure baby has a deep latch! You can learn exactly how to do this by following the steps laid out in this post.
READ MORE: Could your baby have a hidden tongue tie? This is a big reason some babies can’t get a deep latch, and it’s often missed by providers!
3. Adjust baby’s positioning
Sometimes we can help heal sore nipples simply by adjusting how baby is positioned at the breast.
Most babies will have trouble latching on deeply if their body isn’t properly oriented to the breast. Here are a couple things to keep in mind when positioning baby at the breast:
- Make sure you bring baby to the breast. In other words, position baby at the level of your breast rather than hunch over to bring your breast to baby. This will be more comfortable for you and give baby’s body more support.
- Make sure that when baby is at the breast, his or her ears are in line with his or her shoulders, and his or her shoulders are in line with his or her hips. In other words, you shouldn’t see any rotation in baby’s neck or torso. (Note: it is normal for older babies to twist and turn while they feed; this alignment is more important for newborns and younger babies)
- Baby should always be belly to belly with you. When baby is placed belly to belly with you, there is light pressure against baby’s chin, torso, hips, legs and feet, and this pressure triggers inborn feeding reflexes that help baby latch on and breastfeed well. Babies don’t feed well on their backs, so depending on the feeding hold you’re using, adjust baby so that his or her belly is against your belly (or your side, if you’re in a football hold).

4. Try a laid back breastfeeding position
Laid-back breastfeeding helps heal sore nipples by making it easier for baby to latch on well.
Breastfeeding parents who have never taken a breastfeeding class before usually adopt this feeding position because it’s a very natural and comfortable position to feed in for both you and baby. It doesn’t require complicated or specific ways of holding baby, baby is easily well supported, and it allows your baby to use his innate reflexes to achieve a latch that naturally tends to be deeper and more comfortable. It also doesn’t require special breastfeeding pillows, which is nice.
In this position, you want to be lying back far enough that baby can lie on your chest without rolling down your body, but not so far back that you’re lying flat. You can learn more about laid-back breastfeeding (including how to make adjustments to your positioning) here.
READ MORE: 3 Ways To Make Laid-Back Breastfeeding Work For You
5. Try a different feeding hold
If the hold you’re using isn’t helping you get a deep latch, try a new one! While the traditional cradle hold is what you probably most often see, it isn’t actually a great hold for newborns. In the cradle hold, baby’s head rests in the crook of your elbow, which limits your ability to guide baby’s head to your breast. A laid-back, football, or cross-cradle hold may be a better choice.

6. Use moist wound healing to treat damaged nipple tissue
When breastfeeding parents encounter sore nipples, one of the first recommendations you’ll hear in mom groups online is to use nipple cream. But nipple cream is #6 on my list for a reason! Unfortunately, even the world’s best nipple cream won’t fix a poor latch. Nipple creams only treat skin damage: They don’t fix the underlying cause of that damage, and they don’t do anything to make a poor latch less painful!
We used to recommend that breastfeeding parents “air dry the nipples” when treating nipple damage, but we know now that advice is outdated. Dermatologists agree: The best way to expedite healing of damaged skin is moist wound healing. Keeping the nipples moist (with nipple cream or even expressed breastmilk) speeds up epithelial cell regrowth, and wounds heal faster.

(The only time you would not want to keep the nipples moist is if they are shiny and itchy due to a yeast infection. This type of infection is often characterized by shooting breast pain. If you suspect you have a yeast infection on the nipples, meet with your doctor for treatment.)
A Note About Lanolin: Lanolin may not be the best choice for moist wound healing, even though it is frequently suggested and offered. There is some evidence that it can increase the risk of skin infection (source) and it should not be used if you have a wool allergy. If you do use it, a little goes a long way: A small smear on the nipple is usually sufficient.
What about nipple shields?
Nipple shields aren’t my go-to recommendation for managing sore nipples, and here’s why:
First, if your nipples are already sore or damaged, a nipple shield is not necessarily going to prevent pain. You may find that the shield rubs against damaged nipples, or that baby clamps down on the nipple shield the same way he or she may have been clamping down before, which caused the pain to begin with.
Second, babies who cannot latch well/comfortably (or at all) without a nipple shield might have underlying latch issues that can cause low milk supply over time. In other words, it’s unlikely that modern, thin, silicone nipple shields will cause low milk supply, but latch issues that necessitate the use of nipple shields can cause low milk supply.
It might be best to think of a nipple shield as a temporary solution to use while you actively seek out breastfeeding help. You don’t want reliance on a shield to be the reason you delay correcting an underlying latch problem that could cause milk supply issues down the road.
Important Note: If your baby cannot latch at all without the aid of a nipple shield, this is a sign that a lactation consultant should evaluate baby.

What about switching to pumping (temporary or exclusively)?
Sometimes, a temporary switch to pumping can give your nipples time to heal. But in the meantime, if you haven’t taken steps to solve the underlying latch issue that caused the pain to begin with, temporarily switching to pumping might only delay you from getting the help you need!
Plus, pumping is not always risk-free: Not everyone responds well to a pump, and if the pump doesn’t drain your breasts sufficiently, you can experience milk supply issues over time.
That said, there is nothing wrong with needing or choosing to pump! Pumping is simply a tool in our toolbox. And temporary or exclusive pumping is a good choice for many parents! If you decide to move to exclusive pumping, be sure that all bottles are pace fed (this is *extremely important*).
You got this!
Remember, some nipple discomfort in the beginning—the first 1-2 weeks—is normal. Your nipples have probably never experienced these sensations! And even if you’ve breastfed before, your nipples have never nursed this new baby who is breastfeeding for the first time. Don’t be alarmed if you experience nipple soreness. Take the steps listed above instead!
If you enjoyed this post, be sure to check out our digital library of helpful resources that quickly teach how to avoid common breastfeeding problems and give you the peace of mind and confidence you need to meet your breastfeeding goals.