Breastfeeding After A C-Section or Induction: How to Set Yourself Up For Success
This post may contain affiliate links (see full disclosure). As an Amazon Associate, I earn from qualifying purchases.
Are you wondering if breastfeeding after a C-section or induction is going to be more difficult? Birth is rarely predictable, but knowing these recommendations will help maximize your ability to breastfeed after a more complicated birth.
Sometimes you approach labor and delivery knowing things might be a bit complicated. With my first baby, I knew I would be having a C-section. My pregnancy was high risk, and baby was in a breech position (feet down). With my second baby, I planned to attempt a VBAC, and I went into my third trimester very aware that I may wind up being induced or having a repeat Cesarean.
If you find yourself in a similar situation, or you just want to be prepared for all possible scenarios, you’ve come to the right place.
As with birth, sometimes there are things we can’t control about our breastfeeding experience. For example, we can’t directly control when our milk increases in volume after delivery. We can’t always control how well baby is able to feed in the first days of life. We can’t be positive baby won’t need to be monitored in the NICU for a bit after birth.
But with the right knowledge and support, you can increase the odds that your breastfeeding goals will be met, regardless of what happens.

Here’s what you should know about breastfeeding after a c-section or induction:
Medical Disclaimer: The content of this blog post is not medical advice nor is it a substitute for medical advice, diagnosis, treatment, or professional lactation care. This post is for educational and informational purposes only. It is the reader’s responsibility to review all information regarding any medical condition or treatment with a healthcare provider.
PUT BABY SKIN-TO-SKIN WITH YOU AS SOON AS POSSIBLE
Skin-to-skin contact (SSC, sometimes referred to as “kangaroo care”) after birth is immensely beneficial, regardless of whether or not you plan to breastfeed. SSC helps regulate baby’s body temperature, heart rate, breathing and blood sugar levels (source). In fact, unlike the male chest, female breasts automatically cool down or warm up according to baby’s body temperature needs (source)!
If you’re planning on breastfeeding after a C-section, ask your OB about allowing skin-to-skin contact in the operating room. If this won’t be possible, make it known that you wish baby to be put skin-to-skin on your chest as soon as possible after birth. And in the meantime, make plans for your partner or support person to hold baby skin-to-skin early on in case you won’t be able to.
Pro-Tip: The benefits of SSC don’t stop after birth: In babies, SSC is associated with stronger immune systems, improved weight gain, and reduced crying. For you, SSC is associated with reduced postpartum bleeding, a lower risk of postpartum depression, and improved breastmilk production. You can and should continue putting baby skin-to-skin with you throughout baby’s first year of life and beyond as needed (source). SSC is also very beneficial for fathers, as it can help promote attachment (source).

AIM TO BEGIN BREASTFEEDING AS SOON AS YOUR SITUATION ALLOWS
If possible, begin breastfeeding within an hour of birth, but don’t stress out if this doesn’t happen!
Starting breastfeeding within this so-called “golden hour” is associated with good outcomes, but that does NOT mean something bad will necessarily happen if you miss it. Many parents go on to breastfeed just fine regardless.
START EXPRESSING MILK EARLY.
If you find yourself in a situation where baby cannot begin breastfeeding for some time (e.g. baby is premature, in the NICU, or is perhaps simply having difficulty latching on), begin expressing milk within 1-6 hours of birth, or as soon as you are able (source, source).
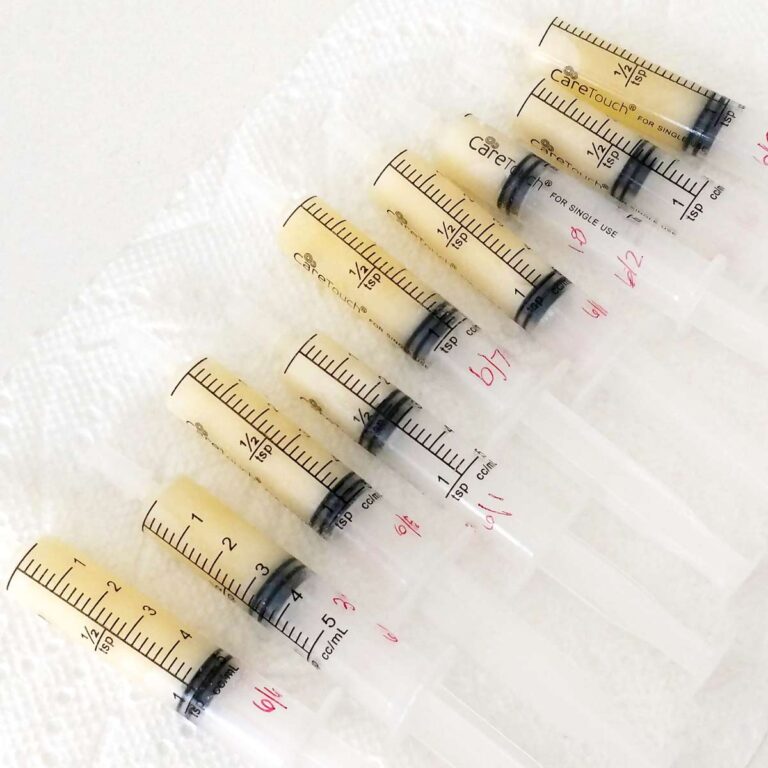
Don’t be surprised if milk only comes out drops at a time! This is normal and expected. This early milk (we call it “colostrum,” but that’s just its fancy name) isn’t very voluminous, but it is very nutrient dense, and baby’s stomach is very small in the first days of life.
Early milk is typically most easily and effectively expressed by hand (source). Otherwise precious drops can get lost in the crevices of your pump’s milk collection bottles. Plus, in the early days, a pump’s suction alone may not be as effective at removing milk as actual breast compressions (source, source, source).
You can watch a video of how to hand express milk here — it’s a good skill for everyone to develop. You can collect the expressed milk in a small, clean container or spoon.

After hand expressing, it is a good idea to also pump both breasts with a hospital-grade double electric pump for about 20 minutes (source, source).
This is because the pump provides a different type of stimulation than hand expression (source), and this extra stimulation can help establish a robust milk supply. Don’t worry if pumping does not yield much extra milk. Remember that right now, the primary purpose of pumping to provide this extra stimulation. Massaging while you pump is always a good idea and usually results in greater milk output (source).
MAKE SURE YOU’RE USING THE RIGHT BREAST SHIELD SIZE.
You’ll know you have the right breast shield size if your nipple can move freely without rubbing against the sides of the shield. At the same time, you don’t want too much of your areola (the darker skin surrounding your nipple) being pulled too far into the pump, either.
This matters because using the wrong breast shield size can decrease how effective your pump is and how much milk you can pump (source).
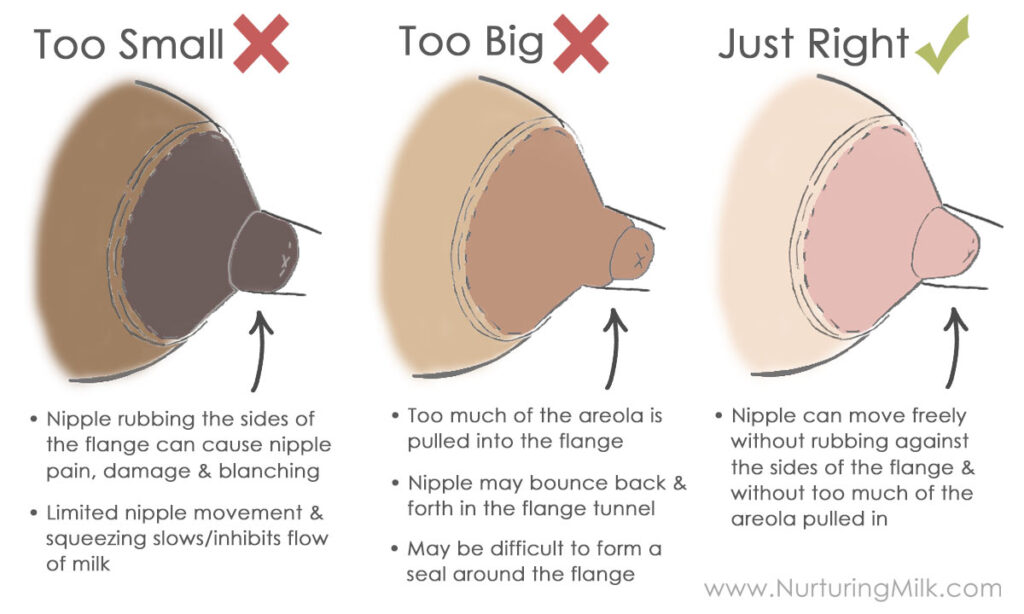
Pro-Tip: If you find you fall in-between shield sizes, or if you see your nipples being stretched far into the shield even with the correct shield size, Pumpin’ Pals inserts or BeauGen pump inserts may help you get a better fit and pump more milk.
If you aren’t able to express much milk—by hand or with a pump—don’t stress. Give baby what you can. Even a little bit is beneficial.
And know that if baby needs to be supplemented with formula, you have not failed. Formula is an important tool for exactly these situations! There is nothing wrong with using tools available to you, and using formula does not mean breastfeeding won’t work out. In fact, formula can be used to support breastfeeding long-term!
BREASTFEED OR EXPRESS MILK AT LEAST 10 TIMES IN 24 HOURS.
If you have the opportunity to breastfeed baby directly, ask if your facility has a lactation consultant (IBCLC) who can assist you. But if you can’t breastfeed directly yet, continue to hand express followed by 20 minutes of pumping both breasts.
Aim to express milk at least 10 times in 24 hours. The hospital may recommend 8 times in 24 hours. This may be sufficient. However, 10 times in 24 hours may be a safer bet. This is because the goal is to pump as often as a newborn would otherwise nurse. Many newborns nurse more often than 8 times in 24 hours. Nursing or pumping more frequently can also help your milk increase in volume up to 24 hours sooner (source).

Ultimately, focus on doing what you can. You just had a baby, and your mental heath matters too. If pumping 8 times in 24 hours is all you can handle, or if you want to change your breastfeeding goals to include formula, you can do so!
PUMP EVERY TIME YOU NEED TO SUPPLEMENT WITH FORMULA
If your baby is able to breastfeed but needs to be supplemented while in the hospital, ask if you can supplement with your own expressed milk before supplementing with formula. Your baby’s doctor or nurse might not mention that this is an option, but it usually is.
If your milk has not yet increased in volume (this typically happens on day of life 3-4), hand express your early milk followed by pumping both breasts for about 20 minutes. If you’ve noticed that your milk has already increased in volume, massage your breasts for a couple minutes, then pump both breasts for about 20 minutes. When pumping, always massage the breasts for best results.
If you don’t have enough expressed milk to supplement with, no worries! Give baby what you have and make up the difference with formula.
You may have heard that giving formula can cause low milk supply down the road, and this is technically true. However, if you pump a full session (about 20 minutes) every time baby receives a bottle of formula, you send your body a signal that it needs to keep producing milk. This helps protect your supply. From this point on and at any point in the future, you will want to make sure you pump a full session any time baby has formula or frozen breastmilk.

CONSIDER AN ALTERNATE FEEDING METHOD WHEN POSSIBLE.
To support breastfeeding, you may consider delaying the introduction of a bottle to baby. Early milk can actually be fed by spoon, cup, or syringe! If you need to supplement with expressed milk or formula, feeding by a device other than a bottle may be helpful and is pretty easy. Ask your nurse or hospital’s lactation consultant for assistance.
MAKE SURE ALL BOTTLES ARE PACE FED.
If a bottle becomes necessary, make sure every bottle is pace fed. Paced bottle feeding is super important, especially for newborns, but it often does NOT happen in hospital settings. You may have to request it or ensure that the person feeding baby is in fact pace feeding.
If you want to learn more about why paced bottle feeding is so incredibly important, I dedicated an entire blog post to it! You can read it here.

SEE AN IBCLC FOR MORE SUPPORT
As I mentioned, you’ll want to ask to see an IBCLC in the hospital if possible. But if the hospital IBCLC doesn’t provide the help you’re looking for, don’t be afraid to seek help elsewhere.
IBCLCs in private practice are sometimes better equipped to provide assistance, often for the simple reason that they have more time to work directly with you than a hospital setting allows. Many private practice IBCLCs are able to meet with you in the comfort of your own home.
Lactation consultants can be a bit like therapists: Not every person is going to connect with you on the right level. It’s very important to find an IBCLC who makes you feel supported, and a good IBCLC will support you no matter how you choose to feed your baby.
Birth complication don’t have to prevent you from reaching your breastfeeding goals.
To recap, if you anticipate that you might have a more complicated birth, knowing these recommendations can help make the transition too breastfeeding a lot easier. It can help establish your milk supply and protect it down the road.
But it’s also important to remember that your mental health is also important. Only you can know for sure which feeding choices are right for your situation, and if you need to adjust your breastfeeding goals, it is okay!
If you enjoyed this post, be sure to check out our digital library of helpful resources that quickly teach how to avoid common breastfeeding problems and give you the peace of mind and confidence you need to meet your breastfeeding goals.